Keywords
Community-Acquired Pneumonia, Lebanon, Refugees, Etiology, Case-Control Studies, Epidemiology, Prevention & Control, Risk Factors
Community-Acquired Pneumonia, Lebanon, Refugees, Etiology, Case-Control Studies, Epidemiology, Prevention & Control, Risk Factors
Lower respiratory tract infections (LRTI) are the second leading cause of mortality worldwide, accounting for an estimated 2.8 million deaths annually, and mainly affect children in developing countries1. Community-acquired pneumonia (CAP) is caused by a variety of bacteria and viruses and is mainly characterized by lobar or broncho-pneumonic changes. However, identification of the etiology of pneumonia is often difficult, and optimal prevention and treatment strategies for CAP critically depend on a full understanding of its etiology. For example, intracellular (“atypical”) bacteria (Chlamydophila, Mycoplasma, etc.) require treatment with specific antibiotics, while purely viral infections do not. Furthermore, clinical exams, chest radiology and biological tests lack specificity, and blood cultures yield positive results in only 10 to 20% of cases.
Current interventions for CAP are primarily based on etiological studies conducted in the early 1980s2–4, which indicated bacteria are responsible for almost half of all cases of CAP5,6; Streptococcus pneumoniae, Haemophilus influenzae and Staphylococcus aureus were the most commonly identified bacteria. In children < 5-years-old, bacteria were responsible for severe forms of CAP: S. pneumoniae and H. influenzae accounted for approximately 60% of cases of severe and fatal pneumonia7,8 and S. pneumoniae alone accounted for 11% of mortalities overall in children < 5-years-old9. However, other bacteria (e.g. Mycoplasma pneumoniae, Chlamydophila pneumoniae, Legionella pneumophila, Bordetella pertussis, etc.) may be responsible for a significant proportion of CAP10. Moreover, respiratory viruses such as influenza viruses, respiratory syncytial virus (RSV) and human metapneumovirus (hMPV) are known to make significant, often seasonal, contributions to CAP. Finally, superinfections, although poorly understood, are widely accepted to contribute to severe CAP. A clear picture of the etiology of CAP would help to estimate the potential impact of novel public health interventions, such as antiviral therapies in case management or influenza vaccination for prevention in vulnerable populations. In order to provide up-to-date data on the etiology of CAP, several studies were recently conducted, in particular two large studies in the USA in 2010–2012, targeting children and adults11,12, and two studies that targeted under-fives in low and middle income countries, the GABRIEL Pneumonia Study in 2010–2014, and the Pneumonia Etiology Research for Child Health (PERCH) study in 2011–201413. These studies pointed to the importance of viruses in the etiology of CAP.
LRTI are a major cause of morbidity and mortality in the acute phase of humanitarian crises. Case management (diagnoses, treatment choice and delivery) and public health interventions (immunization strategies) for CAP in humanitarian crisis settings are conducted blindly or based on the assumption that evidence gathered in non-crisis settings applies to displaced populations. However, large knowledge gaps remain in many areas, including the etiology of these infections14,15. No studies have been specifically designed to assess the etiology of CAP in populations facing humanitarian crisis.
The reference method for identifying the pathogen responsible for an infection is to sample the infected tissues, i.e., the lung, in patients with pneumonia, and screen for pathogenic agents by culture or molecular tools. Such invasive procedures are difficult to set up, even in hospital settings, and virtually impossible in primary health care. To circumvent this issue, the causative agent can be identified using samples from the upper respiratory tract using non-invasive techniques, e.g. nasopharyngeal swabs11,12. Due to the existence of healthy carriers of several potential pathogens (e.g. Streptococcus pneumoniae) in the population, there is a need to adjust for carriage: the higher the proportion of asymptomatic carriers of a given pathogen, the lesser the chances that this agent is the etiology of CAP when found in the upper respiratory tract.
In the last decade, transcriptomic analyses of the blood of patients infected with different pathogens have revealed gene expression patterns that correlate strongly with individual etiologic agents16,17. White blood cells express different genes in response to infection with different agents, and these patterns can be used to distinguish viral and bacterial infections with high accuracy18. These transcriptomic patterns can even distinguish between different viral (or bacterial) infections, and also enable evaluation of the severity of infection. RNA sequencing analysis of the gene expression profiles of white blood cells during infection enables differentiation of viral and bacterial infections with higher specificity than white blood cell counts19. Therefore, transcriptomics represents an innovative tool that reduces the need to identify pathogens by culturing respiratory tract samples and does not need to be adjusted for asymptomatic carriage. The ideal control samples for transcriptomic analysis are samples from healthy patients, i.e. those attending for vaccination or other routine healthcare visits.
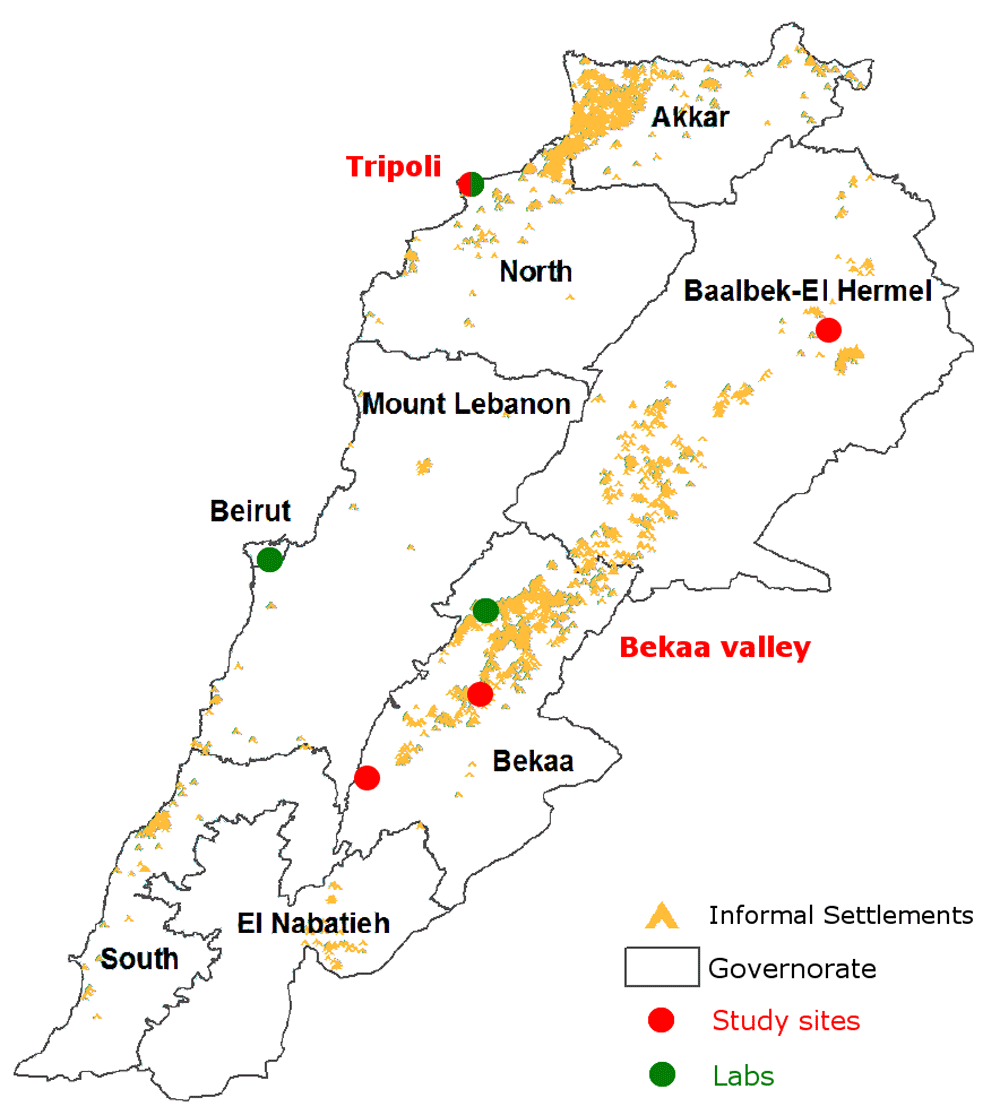
Lebanon is severely affected by a complex, chronic and protracted refugee crisis due to the ongoing war in Syria that began in March 2011. The Bekaa valley is the main entry point for Syrian refugees, followed by the North Lebanon region and Beirut, with refugees settling all over the country. The crisis not only affects Syrian refugees, but also the local Lebanese population and Palestinian refugees who settled decades ago. The majority of Syrian refugees reside in approximately 4000 informal tented settlements and mobile centers, garages and unfinished buildings, with no officially established access to food, water, sanitary means, health or education.
Respiratory tract infections (RTI) are among the leading causes of morbidity and mortality in children and adults affected by the current humanitarian crisis in Lebanon. According to Médecins Sans Frontières (MSF), RTI accounted for at least 56% of ambulatory or in-patient health care visits in the first six months of 2015, and up to 79% of visits among children under 5-years-old in the healthcare facilities attended mainly by refugees in the Bekaa valley (MSF, personal communication). Unpublished data from primary healthcare facilities in Lebanon suggests that 10–25% of these cases of RTI are CAP (Ali Ghassani, personal communication), though data on the etiology and severity of these cases of CAP cases is lacking.
In Lebanon, CAP peaks between October and April. Specifically, 80% of the primary consultations for children during winter are related to RTI, compared to 20% in the summer (Ali Ghassani, personal communication). The Lebanese surveillance program for pulmonary infections due to S. pneumoniae considers the general population, and therefore current data on the incidence, predominant serotypes, and antimicrobial susceptibility of CAP among the refugee population is not available20. UNICEF and the Lebanese Ministry of Health started the introduction of a 13-valent pneumococcal vaccine (PCV) as part of a National Program in 2016, among children of Syrian, Palestinian and Lebanese origin.
In order to fill the knowledge gaps described above, the Pneumonia Etiology Among Refugees and the Lebanese population (PEARL) study was initiated in 2016 to identify the causal pathogenic microorganisms in the respiratory tract of children and adults presenting with signs of CAP to health facilities run by medical associations in the context of a humanitarian crisis. The first inclusions took place in November 2016, and the study is expected to last until March 2018.
The primary objective of the PEARL study is to estimate the population attributable fractions (PAFs) of specific viral and bacterial pathogens, i.e. the proportion of CAP attributable to each pathogen, in both the refugee population and Lebanese population using a combination of conventional methods and transcriptomics. The goals behind this objective are (i) to enable local healthcare staff to provide more accurate diagnoses and improved case management and care, (ii) to help designing antimicrobial stewardship interventions, and (iii) to help assessing the impact of PCV, as it will generate baseline data on the burden of CAP caused by Streptococcus pneumoniae at the introduction phase of PCV in the national vaccination program.
The secondary objectives of the PEARL study are to: identify S. pneumoniae serotypes in nasopharyngeal and blood samples; identify the antimicrobial susceptibility profiles of the pathogenic bacteria isolated from nasopharyngeal and blood samples and compare these profiles with antibiotic prescriptions; examine the association between respiratory viral infections and invasive pneumococcal infections; identify risk factors for CAP in this population, especially those that may be modifiable (crowding, tobacco smoking, domestic sources of smoke produced by cooking or heating, etc.), and thus provide data for prevention programs; provide current data on the incidence and severity of CAP in vulnerable populations in Lebanon; provide a unique transcriptomics dataset as regards the sociodemographic profile of the patients and spectrum of diseases; and assess the operational capacity of rapid, nuclear acid-based point-of-care diagnostic tests in a humanitarian crisis.
Based on refugee density, two main regions were selected for this multicentric prospective case-control study: the Bekaa valley and the city of Tripoli (Figure 1). Both regions have similar demographic composition, dynamics and climate. The population eligible for the study consists of any child (>2-months-old) or adult attending one of four primary healthcare facilities (no hospital facilities) that provide routine health care and immunization: one site located in Tripoli and three sites in the Bekaa valley (Kamed el Loz, Machghara, and Baalbeck El Ain). In addition to refugees, local and vulnerable Lebanese individuals who also attend these health centers (although to a lower extent) will be included for ethical and practical reasons.
Nasopharyngeal, urine and blood samples will be collected from patients with CAP (cases). Adults with CAP able to produce sputum will be asked to provide a sputum sample.
As CAP-related pathogens can also be carried by healthy individuals, control individuals will be recruited from the same health facilities; cases and controls will be matched in a 1:1 ratio by age, season and site. Nasopharyngeal swabs and urine will be collected from all controls; a subset of controls (15%) will also be asked to provide a small blood sample (500–1000 µL) for transcriptomic analysis. Controls will not be asked to provide sputum samples.
Cases. Physicians will evaluate case definitions on the basis of a clinical examination and patient history. Cases should meet all of the following inclusion criteria: (i) patient aged > 2 months, (ii) with cough or dyspnea, (iii) lower chest wall indrawing (in children ≤ 3 years only) or tachypnea, (iv) no wheezing suggestive of asthma at auscultation, (v) onset of symptoms within the last 14 days, (vi) and informed consent statement signed by the patient, parent, or legal guardian (Supplementary File 1). Tachypnea is defined as > 50 breaths per minute in patients between 2-months and < 1-year-old; > 40 breaths per minute, between 1 and < 5-years-old; 30 breaths per minute, between ≥ 5 and <18-years-old and > 20 breaths per minute, if ≥ 18 years-old.
Exclusion criteria are (i) any characteristic of healthcare-associated pneumonia, (including hospitalization at an acute care hospital for 2 or more days within 90 days of infection, residence in a nursing home or long-term care facility, recent intravenous antibiotic therapy, or wound care from medical staff within the 30 days prior to the current infection); or (ii) increased risk of lower airway disease, such as immunocompromised status due to underlying disease, including hemodialysis, or immunosuppressant treatment; or (iii) treatment with inhaled corticosteroids or other asthma medications.
The study nurse will check inclusion criteria, and ask the patient or their parent/guardian to provide signed informed consent and fill in the case report form (CRF), which includes a medical history (e.g. HIV infection, tuberculosis, respiratory infections), risk factors for pneumonia, prior medical treatment and immunizations, description of clinical signs that warrant enrolment in the study, current and recent treatment (antibiotic therapy), disease progression, and socio-economic characteristics (Supplementary File 2). Pulse oximetry is used to assess the severity of CAP22; pulse oximeters will be made available to all four healthcare facilities for the present study and pulse oximetry will be reported in the CRF. Data will be anonymized by attributing a unique patient identification code number issued at enrolment of each patient.
Physicians may request other tests such as chest radiography without interfering with the study protocol. Antimicrobial treatment may begin immediately after blood sampling, if required. Cases and controls may also undergo clinical and lab tests as required. Chest X-ray is not required as this examination is not available at all health care facilities, especially the three remote healthcare facilities in Bekaa valley; if available, results from chest X-rays will be reported in the CRF.
Severity of pneumonia will be classified according to the IMCI/WHO guidelines23. Moreover, in under-fives, we will pay a particular attention to pneumonia with a breathing rate > 50 breaths per minute, assessed twice. This cut-off is higher than the standard IMCI recommendations for children 1–5 years old (40 breaths/min), is more specific for pneumonia24, and was successfully adopted in the ALMANACH protocol25,26.
Controls. An aged-matched control will be recruited for each case by age group (± 1 year for children aged 2 months to 4 years, ± 2 years for children 5–17 years, and ± 5 years for patients aged 18–49 years old and adults aged ≥ 50 years old). Controls will be matched to cases attending the same site in the same calendar month (some flexibility is allowed since controls for cases included at the end of one month may be recruited in the next calendar month). The study nurse will identify next patient consulting for reasons other than respiratory (upper or lower respiratory tract) or gastrointestinal infection, check eligibility, obtain written informed consent from the participant, and fill in the CRF.
Controls should meet all of the following inclusion criteria: (i) patients aged > 2 months attending one of the four sites participating in the study for symptomatic disease or immunization; and (ii) informed consent signed by patient or parent/guardian. Patients will be excluded as controls if they (i) exhibited any symptom of RTI (cough, dyspnea, chest wall indrawing, tachypnea, fever, coryzal symptoms/“cold”) or (ii) intestinal infection (watery/bloody diarrhea, abdominal cramps) in the last 5 days.
As pathogen distributions can vary according to patient age, the univariate and multivariate analyses will be stratified by age group. We calculated the total sample size required for each age group to detect a difference in pathogen prevalence between cases and controls (assuming an equal distribution of samples between the age groups) based on a power of 90% (α = 0.05). Pearson’s χ2 test indicated 150 cases and 150 controls were required in each of the four age strata (2 months to 4 years, 5–17 years, 18–49 years, > 50 years) to detect a 15% difference in pathogen frequency between cases and controls (with a carriage prevalence < 10% in controls) or detect a difference in pathogen frequency of 20% (with a carriage prevalence of up to 30% in controls). If no differences between age groups is observed, pooling the data from age groups will increase statistical power.
Thus, the final sample size will be a minimum 600 cases and 600 controls with the aim of including a maximum of 900 cases and 900 controls.
Biological samples will be collected and stored using standard protocols and transported together with the sample log to the laboratories in a multicentric manner (Table 1). All analytical tests will be performed according to good clinical laboratory practice (GCLP)27 following standard operating procedures defined for the study. Sample processing for cases and controls are illustrated in Figure 2 and Figure 3, respectively.
| Specimen | Collection container | Storage temperature | Assay | Processing | Laboratory |
|---|---|---|---|---|---|
| Blood | Blood culture bottle | +4°C | Blood culture and AST | Real time | CH, LMSE |
| Tempus | +4°C/-20°C | Transcriptomics | Batch | NCH | |
| EDTA tube | +4°C | WBC | Real time | EB, CH | |
| +4°C/-80°C | Triplex PCR | Batch | LRM, LMSE | ||
| Urine | Sterile container (or sterile adhesive bags for babies) | +4°C | Antibiotic activity* | Batch | LRM, LMSE |
| +4°C | Binax | Real time | CH, LMSE | ||
| Nasopharyngeal swab | Viral transport medium | +4°C/-80°C | Triplex PCR | Batch | LRM, LMSE |
| +4°C/-80°C | Micro-array (BioFire)* | Real time | |||
| +4°C/-80°C | S. pneumo CAPS-PCR | Batch | |||
| Nasopharyngeal swab | STGG medium | +4°C | Bacterial culture* | Real time | CH, LMSE |
| +4°C/-80°C | CAPS-PCR | Batch | LRM, LMSE | ||
|
Sputum (adults only) | Sterile container | +4°C | Bacterial culture | Real time | CH, LMSE |
| +4°C/-80°C | Triplex PCR | Batch | LRM, LMSE | ||
| +4°C/-80°C | Micro-array (BioFire)* | Real time | |||
| +4°C/-80°C | S. pneumo CAPS-PCR | Batch |
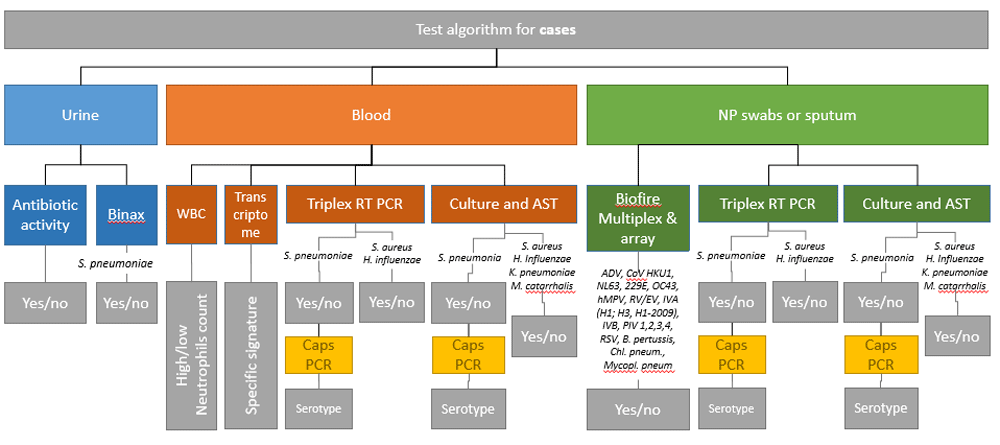
NP, nasopharyngeal; WBC, white blood cells; AST, Antimicrobial Susceptibility Testing; Caps PCR, capsular antigen serotyping PCR.
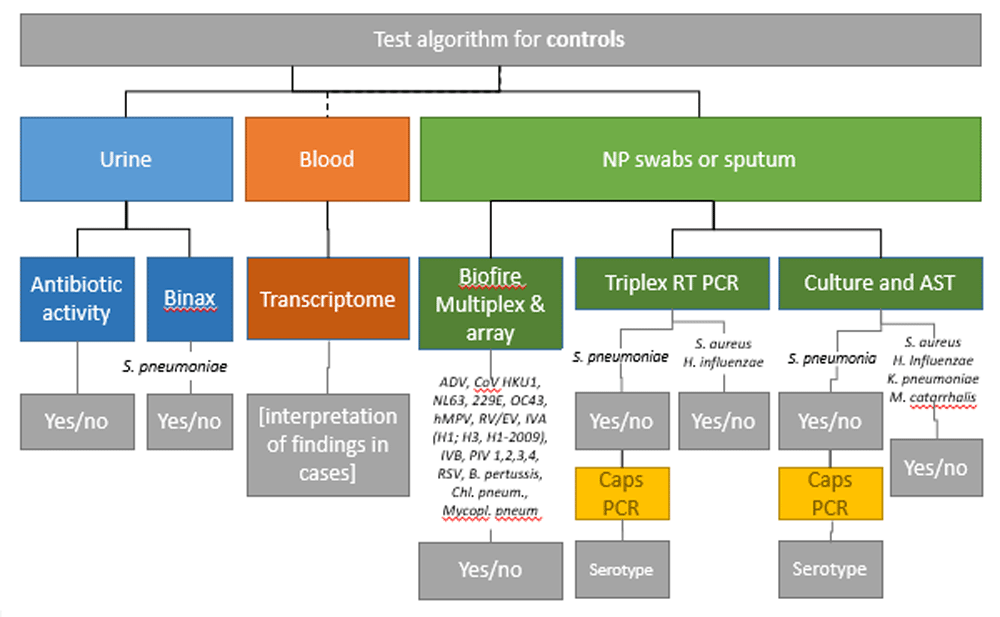
NP, nasopharyngeal; AST, Antimicrobial Susceptibility Testing; Caps PCR, capsular antigen serotyping PCR.
Clinically relevant results will be communicated to the clinicians in a timely manner. Therefore, whenever the lab identifies a pathogen or sensitivity profile of importance for the clinical management of pneumonia, they will provide their etiological diagnosis to the clinical team to ensure appropriate case management. All laboratory data will also be transmitted to the local Fondation Mérieux office in Beirut.
Molecular biology testing of respiratory samples. A trained nurse or lab technician-in-charge will collect two nasopharyngeal samples from all cases and controls28: one will be discharged in virus transport medium (VTM) and the other in skim milk-tryptone-glucose-glycerol (STGG) medium. Nasopharyngeal swabs will be processed and analyzed as shown in Table 1 and Figure 2 and Figure 3.
Nucleic acids extracted from VTM will be subjected to a real-time triplex PCR assay targeting the lytA, vicK and bexA genes29,30 to detect Streptococcus pneumoniae, Staphylococcus aureus and Haemophilus influenzae B, the three most common bacteria detected in CAP.
The FilmArray Respiratory Filmarray (BioFire Diagnostics, Salt Lake City, UT, USA) will be used to identify pathogens that cause pneumonia from VTM31 and sputum samples. The 17 viruses and three atypical bacteria detected by this assay are adenovirus (ADV), coronavirus (CoV) HKU1, coronavirus NL63, coronavirus 229E, coronavirus OC43, hMPV, human rhinovirus (RV)/enterovirus (EV), influenza virus A (IVA), influenza A/H1, influenza A/H3, influenza A/H1-2009, influenza B, parainfluenza virus (PIV) 1, parainfluenza virus 2, parainfluenza virus 3, parainfluenza virus 4, RSV, Bordetella pertussis, Chlamydophila pneumoniae, and Mycoplasma pneumoniae.
Samples from cases positive for Streptococcus pneumoniae by conventional microbiology or triplex PCR will be serotyped using a Multiplex Real-Time PCR assay32 that can identify 40 capsular antigen serotypes (1, 2, 3, 4, 5, 6A/B, 6C, 7C, 7F, 8, 9N/L, 9V, 10A, 10F, 11A, 12F, 13, 14, 15A, 15B/C, 16F, 17F, 18C, 19A, 19F, 20, 21, 22F, 23A, 23B, 23F, 24, 31, 33F, 34, 35A, 35B, 35F, 38, 39) and includes an internal control (LytA).
Culture of bacteria from respiratory samples. Sputum samples and STGG media will be inoculated onto different selective agar plates and incubated under specific conditions (e.g. temperature, CO2) to determine the presence of respiratory pathogens and assess antibiotic susceptibility. Positive cultures will be subjected to Gram staining and examined by light microscopy, and sub-cultured for identification and antimicrobial susceptibility testing if the strain is confirmed to be clinically relevant.
Detection of bacteria in blood. Duplicate aerobic haemoculture assays will be performed for all cases using BacT/ALERT (bioMérieux, Marcy l'Etoile, France) or BACTEC (Becton Dickinson, Franklin Lakes, NJ, USA) automated blood culture systems. If the volume of blood recovered is insufficient to inoculate two bottles, a single culture (6 mL blood) will be performed. Positive cultures will be examined by light microscopy (Gram staining) and subcultured on agar culture media for identification. Antimicrobial susceptibility testing will be performed for all clinically relevant strains.
The semi-quantitative Multiplex Real-Time PCR assay32 will also be conducted on whole blood (EDTA) samples from all cases to identify Streptococcus pneumoniae, Staphylococcus aureus and Haemophilus influenzae B.
Transcriptomics. Blood samples (0.5–1 mL) from all cases and 15% of controls will be subjected to transcriptomic analysis at the Nationwide Children’s Hospital Research Institute, in Columbus, Ohio, USA. Sampling for transcriptomics was initiated in May 2017.
Urinalysis. The presence of antibiotics in urine samples from all cases and controls will be assessed using the disk diffusion method33, and the rapid immunochromatographic Binax® assay (Alere, Orlando, FL, USA) will be used for qualitative detection of S. pneumoniae C polysaccharide antigen in urine34.
All involved healthcare facilities will be required to provide monthly report of the total number of consultations and, whenever available, the number of LRTIs. This will help weighting the monthly results from the study to reflect the actual incidence of CAP.
The primary outcome of the PEARL study is the etiological distribution of CAP, expressed as PAFs for individual pathogenic agents. PAFs will be calculated for each three-month period of the 15-month study, and by patient age group (2 to 11-months-old and 1 to 4, 5 to 17, 18 to 49, and ≥ 50-years-old), by site location (Tripoli vs. Bekaa valley), subpopulation (Syrian refugees versus Lebanese population), and severity of pneumonia.
Additional indicators will be examined to assist data interpretation and for public health and clinical care purposes, including the incidence of RTI and other diseases in the populations consulting the four healthcare facilities involved in the study, agent-specific hospitalization and fatality rates, the socio-demographic characteristics of the patients, clinical signs of CAP (e.g. severity criteria), epidemic features if appropriate (e.g. types of influenza viruses circulating during epidemic periods), and care provided (e.g. antimicrobial use).
All data (CRF, informed consent forms, data logs) will be transmitted to the local Fondation Mérieux office in Beirut for data entry using EpiInfo version 7.2 (CDC, Atlanta, GA, USA). The data will be anonymized by attributing a unique patient identification code number issued at patient enrolment. Access to the names of participants and their corresponding identification codes will be restricted and forms will be secured in locked cupboards.
Data analyses will include (i) descriptive comparisons of the sociodemographic, clinical, and lab data of cases and controls; (ii) univariate/multivariate logistic regression of the relationship between case/control status and pathogens, adjusted for age, season, site, and pneumonia risk factors; and (iii) computation of PAFs for every pathogen, specified by age group, period, study site, subpopulation (Syrian refugees, or general Lebanese population), and pneumonia severity, as described previously35. Analyses will be performed using R version 3.3.2 (R Core Team, Vienna, Austria36) and/or Stata version 13.0 (StataCorp LP, College Station, TX, USA) software. RNA sequencing data from transcriptomics will be analyzed at the Nationwide Children’s Hospital, OH, USA.
The results of the study (microbiological and transcriptomics results) will be published as scientific publications in international peer-reviewed journals. The designation of co-authors will conform to international guidelines governing publications.
The findings of the project, when completed, will be presented to the Ministry of Health of Lebanon, and to the medical and scientific community, such as United Nations agencies and non-governmental organizations, involved in medical care of vulnerable populations in Lebanon. The results will also be communicated via the GABRIEL website (https://www.gabriel-network.org/). The study data relevant to a publication authored by the investigators will be available for review in a public data repository
This study will be conducted in accordance with the Declaration of Helsinki37, the recommendations for Good Ethical Practices in Epidemiology of the Association of French-language Epidemiologists38, the Good Clinical Practice recommendations from the International Conference on Harmonization of Technical Requirements for Registration of Pharmaceuticals for Human Use (ICH) relevant to observational studies39, and the GCLP guidelines of the WHO27. The informed consent statement has been translated into Arabic and was validated during the pilot phase of the study. All adult patients and the parents or legal guardians of children (i.e. ≤18 years) will be asked to sign an informed consent statement prior to enrolment in the study.
As no national ethic committee exists in Lebanon, the study protocol and all other documents related to the trial (informed consent, CRFs, amendments) have been approved by the institutional review boards of the following organizations: El Bashaer Association, Tripoli, Lebanon (5th December 2015); Université Libanaise, Ecole doctorale des Sciences et Technologies, Tripoli, Lebanon (3rd December 2015); Amel Association, Beirut, Lebanon (9th December 2015); and Université Saint-Joseph, Beirut, Lebanon (10th November 2016).
Patient enrollment began in November 2016 and was completed in March 2018. Overall, 1420 patients were included. At the time of submission of the present manuscript, data cleaning and analysis was ongoing.
The Pneumonia Etiology Among Refugees and Lebanese population (PEARL) study will yield unique data on the etiology of CAP in the context of a humanitarian crisis. This study is not only original in terms of target population (refugees), but also as it will assess patients of all ages and adopt a primary health care approach while previous major studies only targeted hospitalized cases2–5,7,13. Therefore, this study may provide a unique and valuable perspective on the etiology of CAP in the context of a humanitarian crisis.
However, assessment of the etiology of CAP in low resource primary health care settings relies on clinical signs for case definition, as chest X-rays are not available at most of the centers in this study. Inclusion criteria for cases of pneumonia are a controversial issue. Several case definitions, based on different clinical, radiological, or biological criteria, have been used in different studies. Opting for a single case definition imposes restrictions on the anatomical and histological levels of the respiratory tract involved, on the severity of disease, and therefore may introduce a bias towards the relative prevalence or contribution of specific pathogens. This makes it difficult to compare results between studies using different case definitions; the present study does not avoid this limitation.
We also anticipate other limitations. For example, the imperfect sensitivity of the diagnostic tests used to identify certain pathogens may result in an underestimation of certain etiological fractions40. Moreover, with regards to surveillance of pneumonia, given that the population covered by the healthcare facilities participating in this study is hard to define, estimation of the precise incidence of CAP in this population might not be possible. Finally, certain aspects of CAP will not be explored in this study, especially AIDS-associated pneumonia and tuberculosis. We expect individuals with HIV will be excluded from the present study as HIV infection is one type of immunosuppression, which is an exclusion criterion. As the prevalence of HIV is very low (< 0.1%) in both the general Lebanese and Syrian populations41, inclusion of cases HIV/AIDS-associated CAP would only have a small effect on the results. Patients with tuberculosis are also expected to be excluded, as cases with symptoms lasting >14 days will be excluded.
Despite these limitations, the PEARL study is expected to provide healthcare planners with an empirical basis for the management of CAP in the context of a refugee crisis. Such information may help to guide population-based health interventions, such as immunization strategies for pneumococci, H. influenzae and influenza. In particular, analysis of S. pneumoniae serotypes in vaccinated and non-vaccinated individuals will provide information on the herd effect following introduction of the PCV in Lebanon and will provide proxy baseline data for evaluation of the success of this vaccination program. This study will also provide practical experience and a methodology for determination of the etiology and involvement of viral and bacterial agents in CAP in other similar humanitarian crisis settings.
No data is associated with this article.
No competing interests were declared by the authors.
The Filmarray® and panels were kindly donated by BioFire Diagnostics, a bioMérieux company. The Institut Mérieux, which is headed by Alain Mérieux and partly belongs to Alain and Alexandre Mérieux, is the main shareholder in bioMérieux. Alain Mérieux is also president of the Fondation Mérieux, and Alexandre Mérieux is on the board of directors of the Fondation Mérieux. Alain and Alexandre Mérieux had no role whatsoever in planning or design of this study. The choice to use Filmarray in this study was made independently of the board of directors of the Fondation Mérieux. Bill & Melinda Gates Foundation, Alain Mérieux and Alexandre Mérieux have had nor will have any role during the execution of this study, or analyses, interpretation of the data, manuscript writing, or decision to submit.
This project is supported by the Bill and Melinda Gates Foundation [OPP1168739] and the Fondation Mérieux.
The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
We would like to thank all of the participants in this study, who provided their time and biological samples. We are very grateful to all health care workers, nurses, medical doctors and laboratory technicians at the participating health facilities, in particular: Ahmad Al Hallak, Anas Altabaa, Ali Rida, Asma Allouch, Danielle Chaaya, Hossam Al Nazer, Hussein Madie, Khaled Hallak, Majdeddine Mouzawak, Marianne Abi Fadel, Maryam Menhem, Nahed Elboosh, Souraya Nasser, Taha Abdou, Yasmine Amraoui, Zeina Jbara, and the other individuals who helped to set up this protocol. Khaled S. Aoun, Kamile, and especially Shafiq Bassil from Bioteck company deserve a special note for their kind collaboration in the transportation of biological samples. We thank Rana Hajjeh, Abdullah Brooks and Keith Klugman for their careful review of the protocol. Editorial support was provided by Andrea Devlin of Science Editing Experts.
PEARL Study Group members: Valentina Abdel Khelek (Amel Association, Lebanon), Mohammad Alabrash (Al-Bashaer Medical Center, Lebanon), Ghadban Al Ghadban (Amel Association), Mohamad Al Zayed (Amel Association), Cynthia Bakkalian (Fondation Mérieux, France), Zeinab Farhat (Amel Association), Ahmad Obeid (Al-Bashaer Medical Center), Pierre Salloum (Bioteck, Lebanon), Haneen Saty (Amel Association).
Supplementary File 1: Informed consent form.
Click here to access the data.
Supplementary File 2: Case report form.
| Views | Downloads | |
|---|---|---|
| Gates Open Research | - | - |
|
PubMed Central
Data from PMC are received and updated monthly.
|
- | - |
Is the rationale for, and objectives of, the study clearly described?
Yes
Is the study design appropriate for the research question?
Partly
Are sufficient details of the methods provided to allow replication by others?
Partly
Are the datasets clearly presented in a useable and accessible format?
Not applicable
Competing Interests: Dr. Howie has a patent 'Lipocalin-2 as a Biomarker for Pneumococcal Infection Status' pending, which is not of specific relevance to this article but of broad relevance to the subject of pneumonia aetiology. No other competing interests were disclosed.
Is the rationale for, and objectives of, the study clearly described?
Yes
Is the study design appropriate for the research question?
Yes
Are sufficient details of the methods provided to allow replication by others?
Partly
Are the datasets clearly presented in a useable and accessible format?
Not applicable
Competing Interests: No competing interests were disclosed.
Alongside their report, reviewers assign a status to the article:
| Invited Reviewers | |||
|---|---|---|---|
| 1 | 2 | 3 | |
|
Version 2 (revision) 13 Jun 19 |
read | read | |
|
Version 1 18 Apr 18 |
read | read | |
Provide sufficient details of any financial or non-financial competing interests to enable users to assess whether your comments might lead a reasonable person to question your impartiality. Consider the following examples, but note that this is not an exhaustive list:
Sign up for content alerts and receive a weekly or monthly email with all newly published articles
Register with Gates Open Research
Already registered? Sign in
If you are a previous or current Gates grant holder, sign up for information about developments, publishing and publications from Gates Open Research.
We'll keep you updated on any major new updates to Gates Open Research
The email address should be the one you originally registered with F1000.
You registered with F1000 via Google, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Google account password, please click here.
You registered with F1000 via Facebook, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Facebook account password, please click here.
If your email address is registered with us, we will email you instructions to reset your password.
If you think you should have received this email but it has not arrived, please check your spam filters and/or contact for further assistance.
Comments on this article Comments (0)